Living with bipolar II often means experiencing emotional highs and lows that feel confusing to both you and the people around you. Unlike its more widely known counterpart, bipolar I, this condition presents with less intense manic episodes, but that doesn't make it any easier to navigate. Many people spend years feeling misunderstood or misdiagnosed before finally learning what's really happening in their brain. If you've ever felt like your mood swings don't quite fit the "typical" description of bipolar disorder, you might be dealing with bipolar II.
What Makes Bipolar II Different
Bipolar II disorder is characterized by a pattern of depressive episodes alternating with hypomanic episodes, rather than full-blown manic episodes. That distinction might sound subtle, but it makes a world of difference in how the condition presents and how it's treated.
Hypomania is the key feature that sets bipolar II apart. These elevated mood states include:
- Increased energy and decreased need for sleep
- Racing thoughts and rapid speech
- Heightened creativity or productivity
- Increased confidence or risk-taking behaviors
- Irritability or restlessness
The catch? Hypomania doesn't typically cause severe impairment in daily functioning or require hospitalization, unlike the manic episodes seen in bipolar I. According to the National Institute of Mental Health, this can actually make bipolar II harder to diagnose because the "up" periods might just seem like you're having a really good week.
The Depression Side of the Equation
Here's something that surprises many people: if you have bipolar II, you'll likely spend way more time dealing with depression than hypomania. The depressive episodes in bipolar II are often severe, persistent, and debilitating. They're not just "feeling down" but can include:
- Profound sadness or emptiness
- Loss of interest in activities you once enjoyed
- Changes in sleep patterns (too much or too little)
- Difficulty concentrating or making decisions
- Thoughts of death or suicide
These depressive periods can last weeks or months, making it easy to see why many people with bipolar II initially get diagnosed with major depression. The comprehensive overview of bipolar disorders explains how the hypomanic episodes might go unnoticed or unreported, especially if they feel good compared to the crushing lows.
Getting the Right Diagnosis
Diagnosing bipolar II requires a careful look at your mood history over time. Your therapist or psychiatrist will want to know about both the highs and the lows, how long they lasted, and how they affected your life.
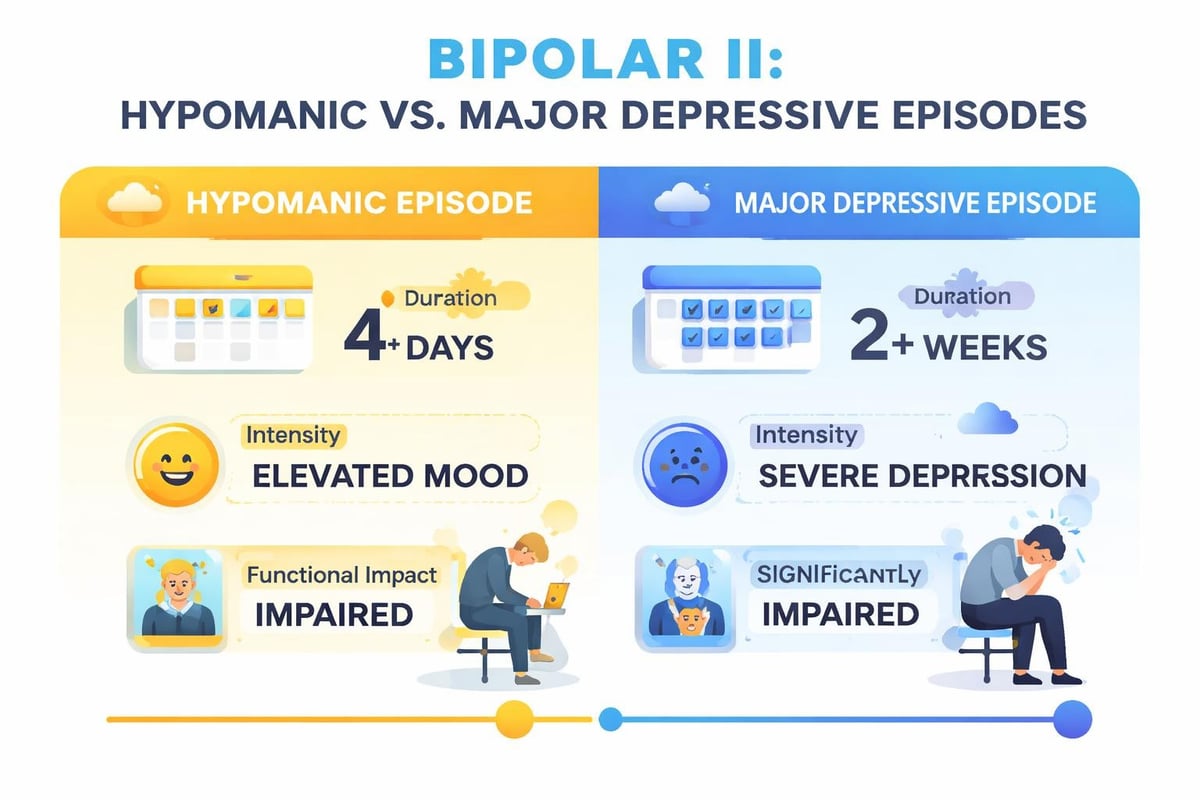
| Mood State | Duration Required | Key Features | Impact on Function |
|---|---|---|---|
| Hypomanic Episode | At least 4 days | Elevated mood, increased energy | Noticeable change but manageable |
| Major Depressive Episode | At least 2 weeks | Low mood, loss of interest | Significant impairment |
| Normal Mood | Varies | Stable emotional state | Full functioning |
One challenge is that people often seek help during depressive episodes and forget to mention the times they felt unusually energized or productive. Be honest with your healthcare provider about those "good" periods too. The detailed clinical features of bipolar disorders can help you understand what information matters most.
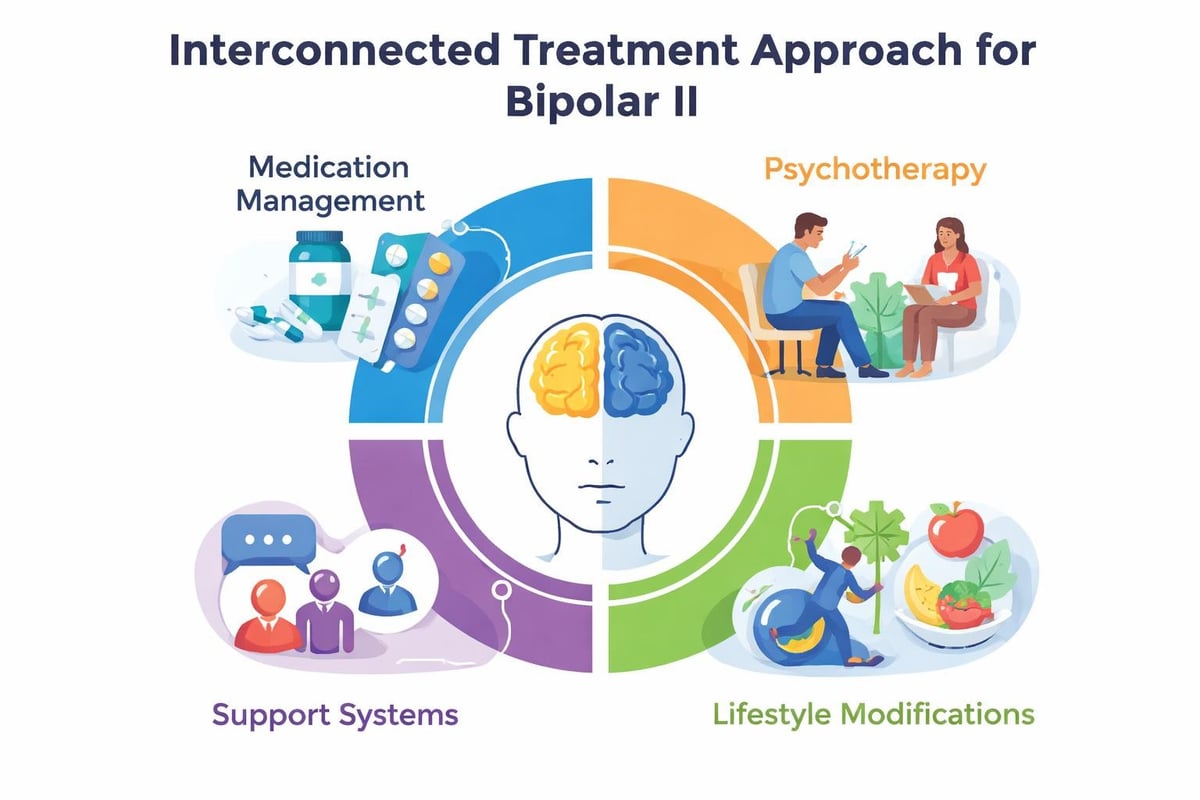
Treatment Approaches That Actually Work
Managing bipolar II effectively usually involves a combination of medication and therapy. There's no one-size-fits-all approach, and what works for your friend or family member might not work for you.
Medication Options
Mood stabilizers form the backbone of bipolar II treatment. These medications help prevent both the highs and lows from becoming too extreme. Some people also benefit from antidepressants, but these need to be prescribed carefully to avoid triggering hypomanic episodes.
Therapeutic Support
This is where evidence-based therapy makes a real difference. At Théla Psychotherapy Clinic, we've seen how approaches like Cognitive Behavioral Therapy (CBT) and Dialectical Behavior Therapy (DBT) help people recognize mood patterns, develop coping strategies, and build emotional regulation skills.
CBT therapy can be particularly helpful for challenging the negative thought patterns that fuel depressive episodes. Meanwhile, DBT skills training teaches you how to manage intense emotions without letting them control your life.
Daily Life with Bipolar II
Living well with bipolar II means developing awareness of your patterns and triggers. You'll learn to recognize the early warning signs of both hypomania and depression, allowing you to take action before things spiral.
Lifestyle factors play a bigger role than you might think:
- Sleep consistency matters enormously (irregular sleep can trigger episodes)
- Stress management helps prevent mood destabilization
- Regular exercise supports mood regulation
- Limiting alcohol and substances prevents additional mood disruption
- Maintaining routines provides stability
Many clients find that tracking their mood, sleep, and energy levels helps them spot patterns they wouldn't otherwise notice. This information becomes invaluable when working with your therapist to adjust your treatment plan.
Building Your Support System
You don't have to manage bipolar II alone. Whether it's individual therapy, support groups, or trusted friends and family, having people who understand what you're going through makes a significant difference.
For those in relationships, couples therapy can help your partner understand bipolar II and learn how to support you effectively without enabling unhealthy patterns.
When to Seek Professional Help
If you're experiencing symptoms that match what we've described, don't wait to reach out for support. Early intervention leads to better outcomes. You should especially seek help if:
- Your mood swings are affecting your relationships or work
- You're having thoughts of suicide or self-harm
- Your sleep patterns have become severely disrupted
- You're engaging in risky behaviors during elevated moods
- Depression is making it hard to function day-to-day
Getting the right diagnosis opens the door to effective treatment. Many people report feeling relieved to finally understand what they've been experiencing and to know that proven treatments exist.

The Path Forward
Recovery from bipolar II isn't about eliminating mood changes entirely (that's not realistic for anyone). It's about reducing the severity and frequency of episodes, developing better coping skills, and building a life that feels meaningful despite the challenges.
With the right combination of medication, therapy, and lifestyle changes, most people with bipolar II can achieve stability and thrive. The journey requires patience, self-compassion, and willingness to stay engaged with treatment even when you're feeling good.
Understanding that bipolar II is a manageable condition, not a life sentence, changes everything. You're not broken or defective - your brain just works differently, and there are effective ways to support it. Whether you're in the early stages of seeking help or years into your treatment journey, know that continued progress is possible.
Understanding bipolar II is the first step toward managing it effectively and reclaiming your life from the unpredictable mood swings. If you're in Ontario and looking for trauma-informed, evidence-based support for bipolar II or other mental health challenges, Théla Psychotherapy Clinic offers both in-person sessions in Markham and online therapy across the province. Our team specializes in CBT, DBT, and other approaches proven to help with mood disorders, creating a safe space where you can develop the skills and insights needed for lasting wellness.

Bonny Li
Contact Me



