In 2026, trauma anxiety depression continue to impact millions of people worldwide, affecting daily life, relationships, and overall well-being. Yet, with new research and expert-backed approaches, there is growing hope for real recovery.
This guide brings together the latest expert strategies and actionable steps to help you understand, manage, and heal from these conditions. You will discover clear definitions, root causes, symptoms, proven therapies, and advances in research.
Explore practical coping techniques and learn about future trends shaping mental health care. Take the first step toward a healthier, more resilient you with guidance grounded in evidence and compassion.
Understanding Trauma, Anxiety, and Depression
Understanding trauma anxiety depression begins with clear definitions and recognizing their unique features. Clinically, trauma refers to the psychological impact of distressing events such as accidents, violence, or loss. Anxiety is characterized by excessive worry and fear, while depression involves persistent sadness and loss of interest. These conditions often overlap, making diagnosis challenging.
A common misconception is that trauma anxiety depression are isolated issues, but they frequently interact. According to DSM-5 and ICD-11, PTSD is a trauma response, generalized anxiety disorder centers on chronic worry, and major depressive disorder involves prolonged low mood. For a deeper dive into trauma and PTSD, visit Understanding Trauma and PTSD.
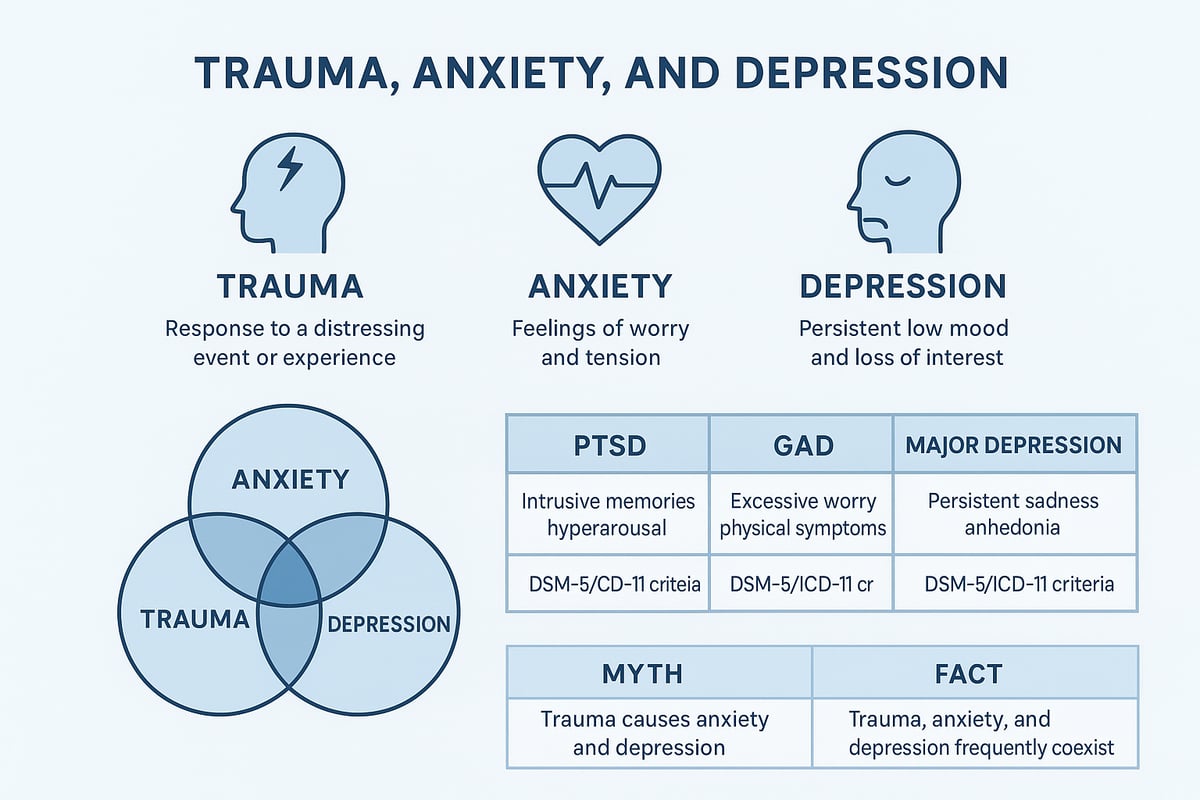
Defining Trauma, Anxiety, and Depression
| Condition | Core Symptoms | Example Diagnosis |
|---|---|---|
| Trauma | Intrusive memories, avoidance | PTSD |
| Anxiety | Excessive worry, restlessness | Generalized Anxiety Disorder |
| Depression | Low mood, loss of interest | Major Depressive Disorder |
Stigma often surrounds trauma anxiety depression, leading some to dismiss symptoms or avoid treatment. However, these conditions can exist together, with overlapping signs such as sleep problems or concentration difficulties. Clinicians use structured criteria to distinguish between them, ensuring accurate diagnosis and care.
Prevalence and Impact in 2026
Trauma anxiety depression remain widespread in 2026, affecting people of all backgrounds. Recent global data from the World Health Organization indicate rising rates, with anxiety and depression now among the top causes of disability worldwide. In Canada, studies from CAMH show increased incidence, especially among youth and marginalized populations.
Demographic trends reveal higher rates of trauma anxiety depression in women and Indigenous communities. The societal impact is significant, affecting workplace productivity, personal relationships, and increasing healthcare costs. For example, the Mental Health of Canadians Report highlights billions lost annually due to untreated mental health issues.
Root Causes and Risk Factors
Multiple factors contribute to trauma anxiety depression. Genetics may increase vulnerability, while brain chemistry and hormonal changes can play a role. Psychological influences such as negative thinking patterns and low self-esteem also contribute.
Environmental stressors, including adverse childhood experiences (ACEs), chronic stress, or exposure to violence, elevate risk. Social determinants like poverty, discrimination, and isolation further compound these challenges. Research consistently links trauma exposure to higher rates of anxiety and depression.
Given the multifactorial nature of trauma anxiety depression, a personalized treatment approach is essential. Addressing both biological and psychosocial factors offers the best chance for effective recovery.
Recognizing Symptoms and When to Seek Help
Identifying the symptoms of trauma anxiety depression is a crucial step toward recovery. Many individuals struggle to distinguish between normal stress and signs that indicate a deeper concern. Early recognition allows for timely intervention, which can make all the difference in outcomes.
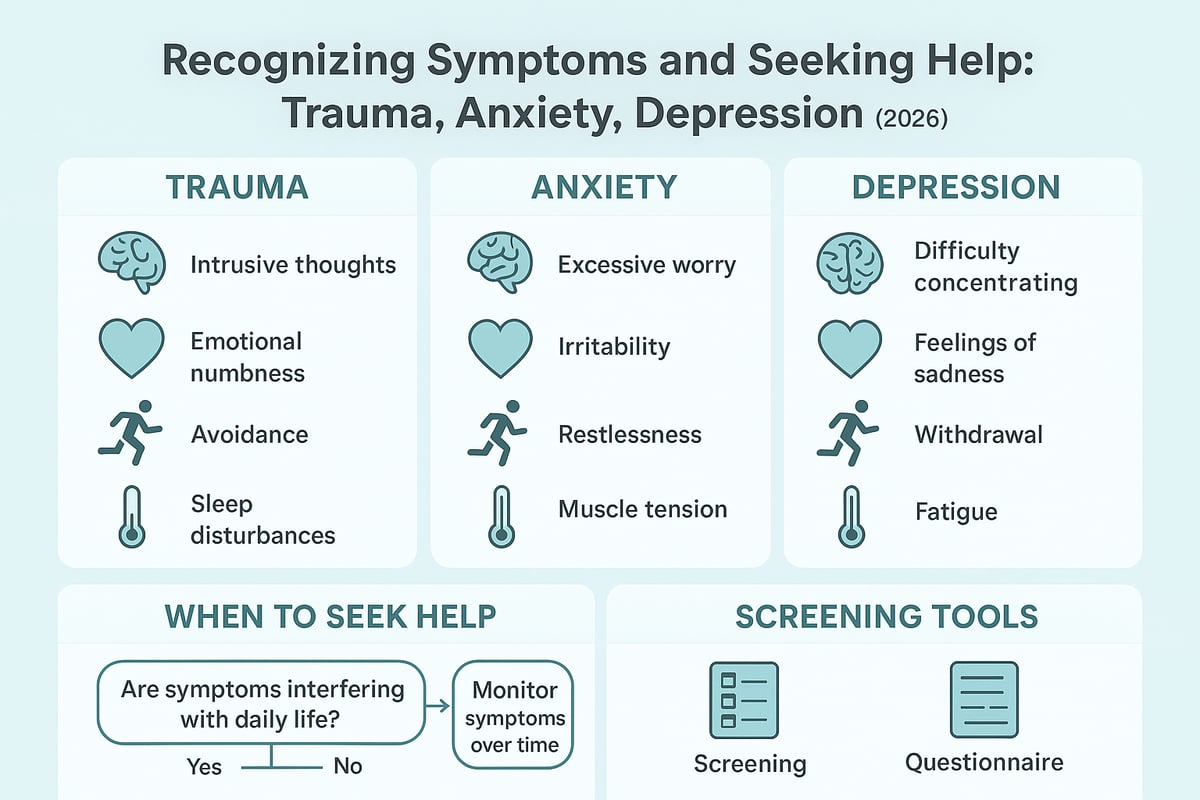
Common Signs and Symptoms
The symptoms of trauma anxiety depression often overlap, making it challenging to pinpoint one condition. Each has unique features, but shared signs can include persistent sadness, irritability, and changes in sleep or appetite.
Emotional symptoms may involve:
- Intrusive memories or flashbacks (trauma)
- Excessive or uncontrollable worry (anxiety)
- Loss of interest or pleasure in activities (depression)
Cognitive symptoms might present as:
- Difficulty concentrating
- Negative thoughts about oneself or the future
- Recurrent doubts or fears
Behavioral symptoms can include:
- Avoidance of reminders (trauma)
- Restlessness or agitation (anxiety)
- Social withdrawal (depression)
Physical symptoms are common, such as headaches, muscle tension, or fatigue.
It is important to note that these conditions can exist together. For example, someone with PTSD may also experience symptoms of generalized anxiety disorder or major depressive disorder. For a deeper dive into how anxiety can present and overlap with other conditions, see Anxiety Causes and Treatments.
Screening and Self-Assessment Tools
Accurate identification of trauma anxiety depression often begins with validated screening tools. Common questionnaires include the PHQ-9 for depression, GAD-7 for anxiety, and PCL-5 for trauma-related symptoms.
| Tool | Purpose | Sample Question |
|---|---|---|
| PHQ-9 | Depression | "Little interest or pleasure?" |
| GAD-7 | Anxiety | "Feeling nervous, anxious?" |
| PCL-5 | Trauma/PTSD | "Repeated distressing memories?" |
These tools are accessible online and in clinical settings. They can help individuals reflect on their experiences and communicate concerns to professionals.
However, self-assessment is not a substitute for a formal diagnosis. The results can guide whether to seek further evaluation but should be interpreted with caution. Only a licensed mental health provider can confirm a diagnosis of trauma anxiety depression, ensuring the right treatment plan is created.
When and How to Seek Professional Help
Recognizing when to seek help for trauma anxiety depression is vital. Red flags that signal immediate attention include:
- Thoughts of self-harm or suicide
- Significant difficulty in daily functioning at work, school, or home
- Substance misuse as a way to cope
In Canada, accessing mental health services in 2026 has become more streamlined. Individuals can start by contacting their primary care provider or connecting with local mental health organizations. Many clinics now offer virtual intake appointments, making support more accessible.
Early intervention greatly improves recovery prospects. For example, a young adult struggling with persistent anxiety and depressive symptoms noticed worsening academic performance. After completing a self-assessment and reaching out to a professional, they began targeted therapy and saw steady improvement.
If you or someone you know is experiencing symptoms of trauma anxiety depression, do not wait. Seeking help is a sign of strength and the first step toward healing.
Evidence-Based Treatment Options for 2026
Advancements in treating trauma anxiety depression have transformed the mental health landscape by 2026. Individuals now have access to a diverse range of evidence-based interventions, many tailored to personal needs and cultural backgrounds.
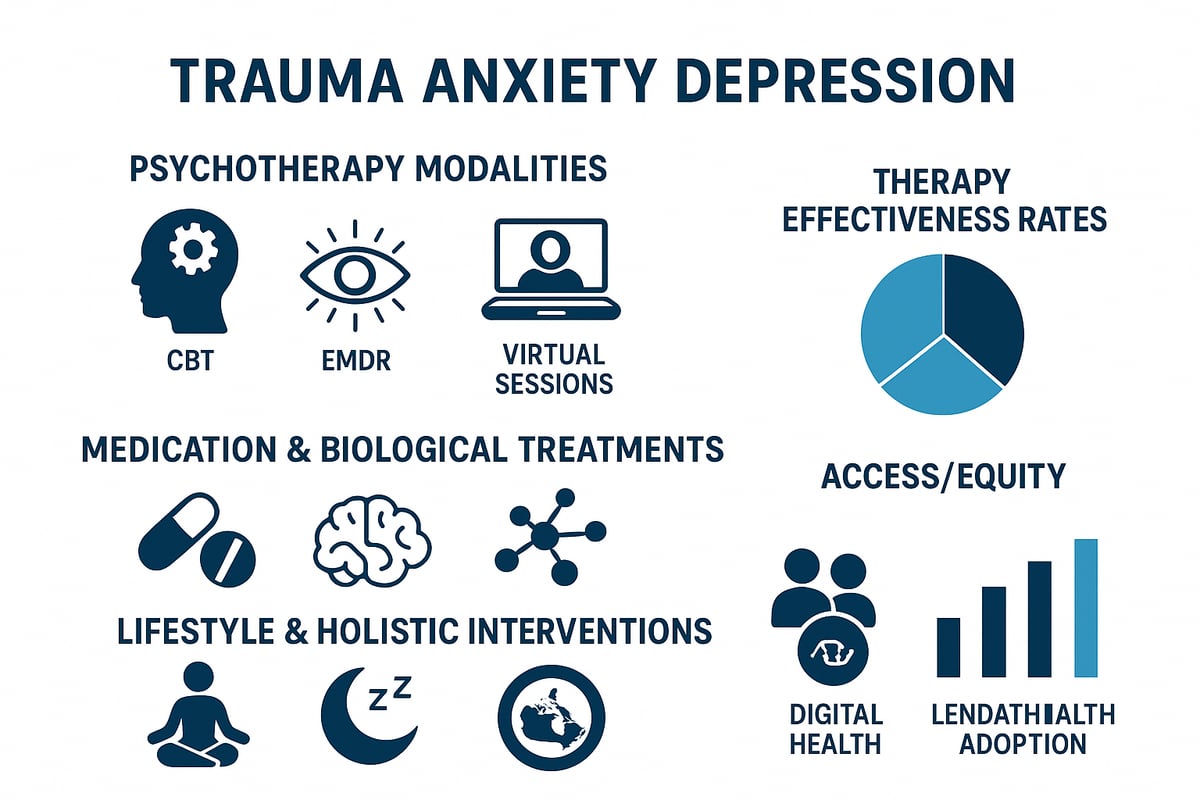
Psychotherapy Modalities and Innovations
Psychotherapy remains the cornerstone of care for trauma anxiety depression, with significant innovations shaping 2026. Cognitive Behavioral Therapy (CBT), Dialectical Behavior Therapy (DBT), Eye Movement Desensitization and Reprocessing (EMDR), and Emotion-Focused Therapy (EFT) have evolved through technology and research.
Digital advancements now allow individuals to access therapy via secure video platforms, AI-powered chatbots, and even virtual reality for exposure treatment. A recent Mental Health Generative AI Study found that AI chatbots effectively reduce symptoms of trauma anxiety depression, offering support between sessions and in underserved regions.
Culturally responsive and trauma-informed care approaches are standard, ensuring therapy is personalized to one's background. Recent clinical trials show improved outcomes when digital tools are combined with traditional therapy, making treatment more accessible and effective for those recovering from trauma anxiety depression.
Medication and Biological Treatments
Medication remains vital for many people experiencing trauma anxiety depression. Newer antidepressants and anxiolytics in 2026 offer improved safety profiles and fewer side effects.
Emerging biological treatments such as ketamine infusions and psychedelic-assisted therapy (including MDMA for PTSD) are now available in specialized clinics. These treatments are closely monitored for effectiveness and safety, providing options when traditional medications are insufficient.
Patients and providers carefully weigh the benefits and risks of each approach, with most protocols recommending medication as part of a comprehensive trauma anxiety depression treatment plan.
Lifestyle and Holistic Interventions
Lifestyle changes are essential in managing trauma anxiety depression. Regular physical activity, balanced nutrition, and quality sleep form the foundation of self-care.
Integrative practices like yoga, meditation, and animal-assisted therapy complement conventional treatments. Data from recent studies confirm that exercise can significantly reduce depressive symptoms and improve anxiety.
Mindfulness and relaxation techniques are widely recommended, giving individuals practical tools to support their trauma anxiety depression recovery journey.
Barriers to Access and Health Equity
Despite progress, disparities in care persist for trauma anxiety depression, especially among rural, Indigenous, and marginalized populations. Access to innovative treatments may be limited by geography, cost, or systemic barriers.
Ongoing policy reforms and community-based programs aim to close these gaps, ensuring equitable access to mental health services for all Canadians.
Practical Coping Strategies and Self-Help Techniques
Finding ways to manage trauma anxiety depression on a daily basis can empower individuals to regain control and foster healing. By integrating practical coping skills, building strong support systems, and preparing for setbacks, recovery becomes a realistic and sustainable goal.
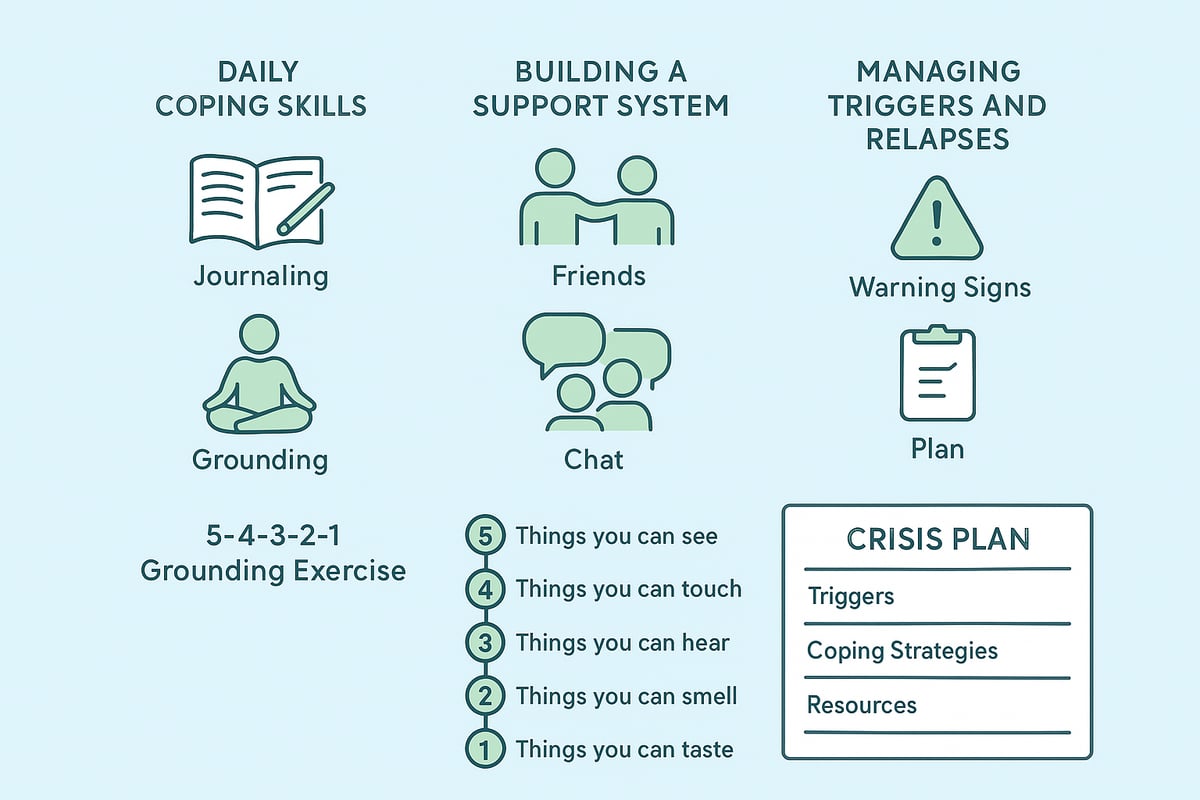
Daily Coping Skills
Daily coping skills are essential for managing trauma anxiety depression. Simple techniques can help calm the mind, improve mood, and break cycles of distress.
Grounding exercises bring attention back to the present. The 5-4-3-2-1 technique is highly effective: Notice five things you see, four you can touch, three you can hear, two you can smell, and one you can taste. This method interrupts overwhelming thoughts and reconnects you to the here and now.
Deep breathing slows the nervous system, while journaling helps process emotions. Mindfulness practices, such as guided meditations, foster self-awareness and acceptance. Self-compassion exercises, like affirmations, can reduce negative self-talk.
If you are looking for structured tools, the Trauma Recovery Starter Kit provides practical resources specifically designed for trauma anxiety depression recovery.
Building a Support System
No one should face trauma anxiety depression alone. Building a reliable support system is a cornerstone of recovery. Friends, family, and peer support groups offer understanding and encouragement, making it easier to share experiences and feel less isolated.
Communicating your needs clearly is key. Let loved ones know how they can help, whether by listening without judgment or assisting with daily routines. Many find comfort in joining online forums or local support groups, where shared experiences foster connection.
Accessing professional and community resources can further strengthen your network. Seeking out both in-person and virtual support options ensures help is available when needed.
Managing Triggers and Relapses
For those navigating trauma anxiety depression, identifying personal triggers is crucial. These might include certain places, people, or stressful situations. Keeping a list of warning signs, such as changes in sleep or mood, can help you recognize when extra support is needed.
Creating a relapse prevention plan is a proactive step. Write down coping strategies, emergency contacts, and steps for self-care. Crisis management tools, including safety planning and helplines, provide immediate support during difficult moments.
Consider using a simple crisis plan template:
Crisis Plan:
- Warning Signs: _______________
- Coping Skills: _______________
- People to Contact: ___________
- Emergency Numbers: ___________
Having this plan on hand can make a significant difference in moments of distress.
Advances in Trauma, Anxiety, and Depression Research
The landscape of trauma anxiety depression research is evolving rapidly. Recent discoveries in neuroscience, digital health, and innovative therapies are paving the way for more targeted, effective interventions. These advances offer new hope for those affected by trauma anxiety depression, promising better outcomes and improved quality of life.
Breakthroughs in Neuroscience and Genetics
Groundbreaking studies are revealing how trauma anxiety depression affect the brain and body. Neuroimaging has identified changes in regions linked to emotional regulation, such as the amygdala and prefrontal cortex. Genetic research is uncovering markers that influence individual vulnerability and resilience, fueling the rise of personalized medicine.
Innovations in biological treatment are also making headlines. For example, new trials are exploring the use of psychedelics and MDMA to treat post-traumatic stress, with the MDMA for PTSD Treatment article highlighting recent FDA reviews. These scientific advances are helping to decode the complex mechanisms behind trauma anxiety depression and guide future therapies.
Technology and Digital Health Solutions
Technology is transforming how trauma anxiety depression is monitored and managed. Artificial intelligence powers chatbots that deliver real-time support, while digital mental health platforms offer evidence-based interventions like cognitive behavioral therapy.
Wearable devices and biofeedback tools now enable symptom tracking and early detection of mood shifts. These innovations make care more accessible, especially in remote or underserved regions. Digital solutions are also helping clinicians tailor interventions to individual needs, improving engagement and outcomes for those coping with trauma anxiety depression.
Future Directions in Prevention and Treatment
The future of trauma anxiety depression research is focused on prevention and precision care. Clinical trials are testing new therapies, including virtual reality exposure and neurostimulation, to enhance recovery. Preventive strategies, such as early screening for at-risk youth and workplace mental health initiatives, aim to reduce incidence and severity.
Global partnerships are driving mental health initiatives, promoting equity and access to care across diverse populations. As science progresses, the integration of genetics, technology, and holistic approaches promises a new era of personalized, effective treatment for trauma anxiety depression.
Navigating Recovery: Building Resilience and Long-Term Wellness
Recovery from trauma anxiety depression is a journey, not a destination. Building long-term wellness means developing resilience, creating a tailored plan, and learning to manage setbacks along the way. These steps offer a foundation for lasting change and improved quality of life.
Developing Resilience and Coping Over Time
Resilience is the ability to adapt to adversity and recover from difficult experiences such as trauma anxiety depression. Key components include optimism, adaptability, and the search for meaning after hardship.
Practical skills training, such as problem-solving and emotional regulation, can foster resilience. Many individuals experience post-traumatic growth, finding new strengths and perspectives after facing challenges.
Longitudinal research shows that survivors who actively engage in resilience-building practices report better outcomes over time. Even small steps, like celebrating progress or maintaining hope, can make a difference for those navigating trauma anxiety depression.
Creating a Personalized Recovery Plan
A personalized recovery plan is essential for managing trauma anxiety depression effectively. Begin by setting realistic, achievable goals. Track your progress, noting both improvements and areas that need adjustment.
Work closely with healthcare providers to ensure your plan reflects your unique needs and values. Regular check-ins allow you to modify strategies as life circumstances evolve. Consider integrating insights from resources such as Depression and Mood Disorders to better understand your symptoms and treatment options.
Remember, an effective plan is flexible. Adjusting your approach is a sign of strength, not failure, in the journey to overcome trauma anxiety depression.
Overcoming Setbacks and Sustaining Progress
Setbacks are a normal part of recovery from trauma anxiety depression. Managing expectations and normalizing occasional difficulties can help you stay motivated.
Use strategies like self-compassion, regular review of your achievements, and seeking support from trusted individuals or support groups. Ongoing education and connecting with mental health resources can reinforce your progress.
Sustaining wellness means committing to long-term self-care and reaching out when needed. With persistence and the right support, long-term recovery from trauma anxiety depression is possible.
As you explore the latest expert strategies for understanding and healing from trauma, anxiety, and depression, remember that you do not have to navigate this journey alone. At Théla Psychotherapy Clinic, we offer a safe, supportive environment—both in person and online—to help you build resilience and achieve lasting wellness. Whether you are ready to take your first step or seeking tailored care that honors your unique story, I encourage you to reach out.
Book Your Free Consultation Appointment Now and discover how compassionate, evidence-based therapy can support your path to recovery.

Bonny Li
Contact Me